
Oct. 12, 2022
Contact: Eric Stann, 573-882-3346, StannE@missouri.edu
Diana Pummill has always struggled with “just sitting around.” So, when she’s not spending time with her husband, Gerry, her children or her grandchildren, she can often be found upcycling — a crafting hobby she developed from a lifelong passion of letting her creativity run wild.
“I do a lot of repurposing,” Pummill said. “I like to take old things that most people would consider as junk and recycle them.”
Pummill, a self-described “country girl” from Otterville in rural, west central Missouri, used to travel to big open-air flea markets in search of the next item to indulge her enthusiasm for upcycling. But two years ago, those trips stopped when she began experiencing health issues.
“I knew something was wrong with me because I hadn’t felt right for a while,” she said. “I guess you could say I was worried, irritated and all of that other thinking that goes along with my situation because I was probably in for some crap, but I knew I would just have to deal with it.”

She was right. In September 2020, doctors at MU Health Care diagnosed Pummill with two different types of cancer — neuroendocrine carcinoma of the gastrointestinal tract and uterine cancer.
But, thanks to recent developments in medical technology, doctors like Greg Biedermann, Pummill’s radiation oncologist at MU Health Care, can utilize targeted approaches to treat different forms of cancer, like an injectable radiopharmaceutical called Lutathera®. By using Lutathera®, which targets the type of neuroendocrine tumor that Pummill’s been diagnosed with, the 62-year-old has already felt a boost in energy when compared to her previous treatments. And with her renewed sense of energy, she has returned to working on her favorite hobby.
Much of Lutathera’s effectiveness is based on its key ingredient, lutetium-177 — a radioisotope produced for this drug in only one location in the United States, the University of Missouri Research Reactor (MURR).
MURR operates 6.5 days a week for 52 weeks a year to produce and distribute radioisotopes like lutetium-177 that are critical to precision medical treatments, diagnostic imaging, and other scientific research and discovery ranging from anthropology to veterinary medicine. The facility’s work with radioisotopes used in medical treatments is critical for cancer patients, said J. David Robertson, executive director of MURR.
“These drugs cannot be stockpiled due to their short half-lives, or their quickly diminishing effectiveness as their active ingredients undergo radioactive decay,” Robertson said. “This means if these drugs are not produced this week, cancer patients will not receive their treatments next week.”
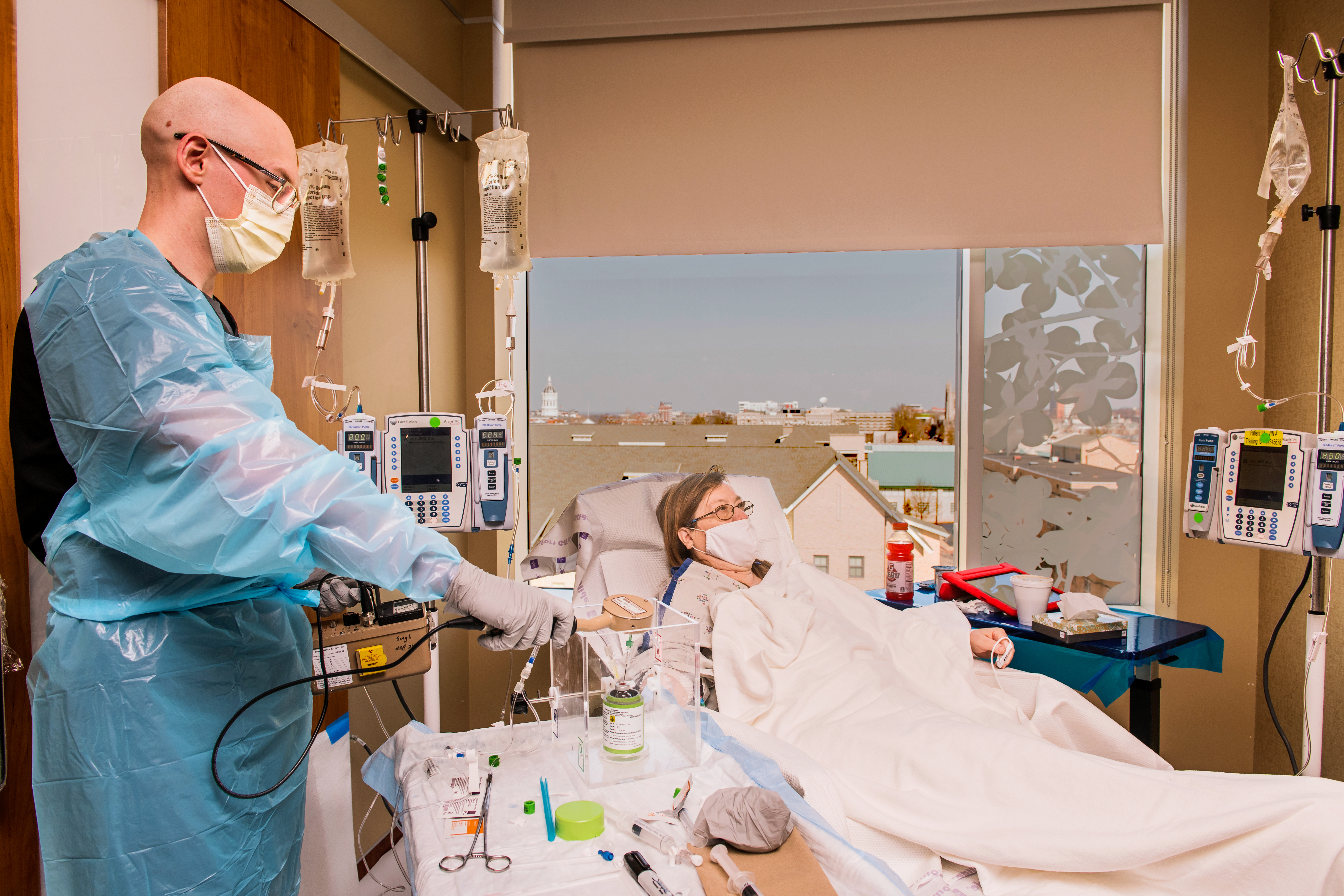
Biedermann said a targeted treatment method like Lutathera® offers an alternative approach to traditional treatments such as chemotherapy because it causes less collateral damage to other parts of the body that are otherwise healthy. While it’s still early in Pummill’s treatment journey to know how she’s doing, he’s optimistic about how well the drug is working for his patient based on past results he’s seen with other patients using Lutathera®.
“Lutathera® has the ability to slow or stop disease progression in patients whose disease has gotten worse on conventional therapy alone,” said Biedermann, who is also an assistant professor of clinical radiology in MU School of Medicine. “Most patients will remain stable for up to three years or more after completing Lutathera®. What’s exciting is that these patients are expected to live longer by several years compared to if they continued with just their conventional treatment. So, we expect that this will give patients [like Pummill] more quality time to spend with their loved ones.”
A team focused on care, now and in the future
Biedermann’s work with patients like Pummill is already helping in the future development of targeted approaches to treat different types of cancer.
“In my day-to-day job, I see patients who are diagnosed with cancer, and I help develop treatment strategies for them,” Biedermann said. “As someone who has experience with the last step of the translational research process, I'm trying to provide some guidance to help lead to some great innovations here at Mizzou.”
That’s why he’s partnered with Carolyn Anderson, a professor of chemistry in the MU College of Arts and Science, and her team on a translational research project working to help move basic science discoveries from the lab to practical application quickly and safely.
“What's beautiful about nuclear medicine is we're taking a radioactive agent and using it for diagnostics such as determining how the body functions, including changes in molecular biology or biochemistry in a diseased state,” said Anderson, who directs the Molecular Imaging and Theranostics Center at MU. “Using a combination of therapy and diagnostics, we can look at how a radiopharmaceutical can be targeted by designing it to go exactly to the place where the disease is located.”
Anderson’s lab and others at MITC serve as a hub for collaborators across the MU campus, scientists from other universities, and industry partners to brainstorm and perform the initial pre-clinical experiments that set the stage for translation into first-in-human studies. The clinical expertise of doctors like Biedermann is an important component as Anderson’s team develops new imaging agents and radiopharmaceutical therapies.
“We are more successful when we have clinician scientists like Dr. Biedermann telling us things like what are the unmet needs, or here’s the problem that we're seeing in treating patients,” Anderson said.
Into the Future
The collective efforts of Anderson, Biedermann and Robertson are supported by MU’s most ambitious research initiative, the NextGen Precision Health initiative.
Highlighting the promise of personalized health care and the impact of large-scale interdisciplinary collaboration, the NextGen Precision Health initiative is bringing together innovators from across MU and the UM System’s three other research universities in pursuit of life-changing precision health advancements, just like using Lutathera® for the treatment of neuroendocrine carcinoma in patients like Pummill. This significant, collaborative effort leverages the research strengths of MU and teams like the one led by Anderson to provide a better future for the health of Missourians and beyond.

Today, Pummill is back to making items such as birdhouses, key holders, wreaths and wind chimes out of old license plates, bicycle wheels and other materials. She hopes her treatment journey with MU will benefit others struggling with similar issues.
“I thought, I’ve got to do something, and if I can help others with getting this figured out as well, maybe it will help them enjoy life more, too. Throughout it all, the people at Mizzou have been good to work with,” she said.
To learn more about this research, visit: At the forefront of nuclear medicine



